Recognising the visible features of Marfan syndrome is a route to identifying the condition’s invisible, potentially deadly feature - the ballooning aorta. This is Marfan syndrome’s dark secret, one that must be exposed before it’s too late. There’s a life-threatening gulf between early and late diagnosis of Marfan syndrome and it’s imperative that the undiagnosed do not remain overlooked. John (not his real name) wrote to share his story, of how he was caught only just in time.
“I was born in 1970 and only diagnosed as having Marfan syndrome in 2010, a few years before I had life-saving heart surgery for a condition that would have gone undiagnosed. I can say that with some confidence, as I approached my GP and asked about Marfan in 2007, as directed by a physio I was being treated by for an unrelated condition. My GP laughed and said 'Oh yes, physios love to think they have found a Marfan patient'. Three years later my son was born with a dislocated lens in one eye. His doctors asked me if I had heard of Marfan syndrome and I said 'Yes'. A genetics test confirmed their suspicions and my diagnosis also.
I still find it hard to believe that I was missed. I am over 1.5 feet taller than my parents. I have long fingers and curled toes, a short body with long arms and legs. My eyesight is terrible, I have curvature of the spine and am extremely loose-jointed. This is why the work of organisations such as yours is so important. So that more parents will get access to life saving treatment that will allow them to see their children grow old. Thank you for the work that you do.
Signs and Symptoms of Marfan Syndrome
The syndrome manifests in different and disparate ways which makes it difficult to diagnose.
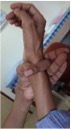
SKELETON: musculo-skeletal problems are common and troublesome in MFS, with Marfan patients often growing to excessive height with long fingers and hammer toes while developing curvature (scoliosis/kyphosis/lordosis) of the spine. Skeletal problems also involve abnormally shaped chest (pectus deformity) and loose joints, often causing pain and dislocation.
- Recognition from a RHEUMATOLOGIST could be the first vital step towards diagnosis of the underlying condition.
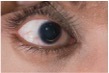
EYES: people with Marfan syndrome are generally myopic, with some experiencing dislocation of the ocular lens and retinal detachment. Strabismus (squint) and glaucoma are also ocular signs.
- Recognition from an OPTICIAN is sometimes the first vital step towards diagnosis of the underlying condition.
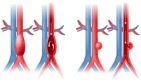
HEART: Ballooning and potentially fatal tearing of the aorta and backward billowing of the heart’s valves. These features can cause death at an early age unless diagnosed in good time and treated medically and surgically. Doctors must listen to the heart and send patient for an echocardiogram.
- Recognition from a CARDIOLOGIST is a path to diagnosis.
DENTAL: A high-arched palate and crowding of teeth with a history of tooth extraction.
- Recognition from a DENTIST is another a route to diagnosis of Marfan syndrome.
SKIN: The lack of elasticity skin in Marfan syndrome means that patients often develop stretch marks and loose sagging skin.









